Washington HIX
Washington Healthplanfinder is the state's official online health insurance exchange that connected 1.5M+ individuals, families, and small businesses to affordable insurance plans and financial assistance under the Affordable Care Act ("Obamacare").
When a life event triggers new health coverage needs, how do you let people act before the system can verify?

ROLE
Product Designer & Product Manager
CLIENT
Department of Health & Human Services, Washington
TEAM
Engineering
QA
Business Owners
Policy Experts
Compliance
Legal
METHODS
Impact Analysis
Stakeholder Interviews
Wireframes
UAT
Timely, affordable coverage that adapts to life's changes
Healthplanfinder is Washington's official affordable health insurance marketplace that served 1.5M+ residents.
Outside annual open enrollment, qualifying life events (e.g., marriage, childbirth, job loss) trigger Special Enrollment Periods that let residents access coverage mid-year. Eligibility requires document proof, but that process of verifying was manual and kept eligible people uncovered for months.
As product designer and product manager, I led the design of how the system handles qualifying-event verification by introducing a new lifecycle state – "conditional enrollment." The result: faster time-to-coverage for customers and fewer manual hours per case for account workers.
PROBLEM
The pre-existing process handled this sequentially: a resident mailed in documents, an account worker reviewed them, and only upon approval could a customer enroll in a plan.
Account workers manually processed every case, which created a bottleneck that became unsustainable with demand.
After a major life change (like losing a job or having a baby), customers needed new health coverage fast. However, the only way to verify eligibility was by mail or in person, delaying coverage by up to 90 days.
Conditionally enrolled status
Customers can pay their first premium and enroll in a plan before verification completes. The platform withholds payment from the carrier until documents are approved, then releases it and activates coverage.
Document status tracking
Document processing status shows up on customer dashboard (e.g., "document uploaded", "verified", etc.)
Retroactive coverage
Account workers can backdate coverage dates based on verification date and case-by-case exceptions per policy.
SOLUTION
I designed the online document upload and verification flows while introducing a new lifecycle state – "conditionally enrolled."
For customers, they can:
-
Upload required documents directly via portal
-
Enroll and pay for a plan upfront, pending verification
-
Track document status in real time
For account workers, they can:
-
Access pending cases in a queue with filters
-
Review, flag, and approve documents

Document processing statuses provided visibility for to customers and account workers about a pending case.
We also gave account workers the ability to filter, sort, and query cases by status so they can prioritize most urgent cases.

HOW WE GOT THERE
While streamlining the document verification process, the idea of conditional enrollment emerged to minimize the a bigger problem of a coverage gap.
The original goal was to digitize document verification to reduce processing delays. However, Account Workers still had up to 30 days to approve a document, and plan selection and enrollment were still gated by approval. For the residents who depended on the platform for affordable healthcare, that hindered their ability to plan for care.
Planning for the worst case in queues, I proposed a conditional enrollment state: users select and pay for a plan upfront, while coverage activates retroactively when verification clears.
Enrollment and payment now happen in parallel with document review, so customers no longer have to wait for documents to be reviewed before they can select and pay for a plan.
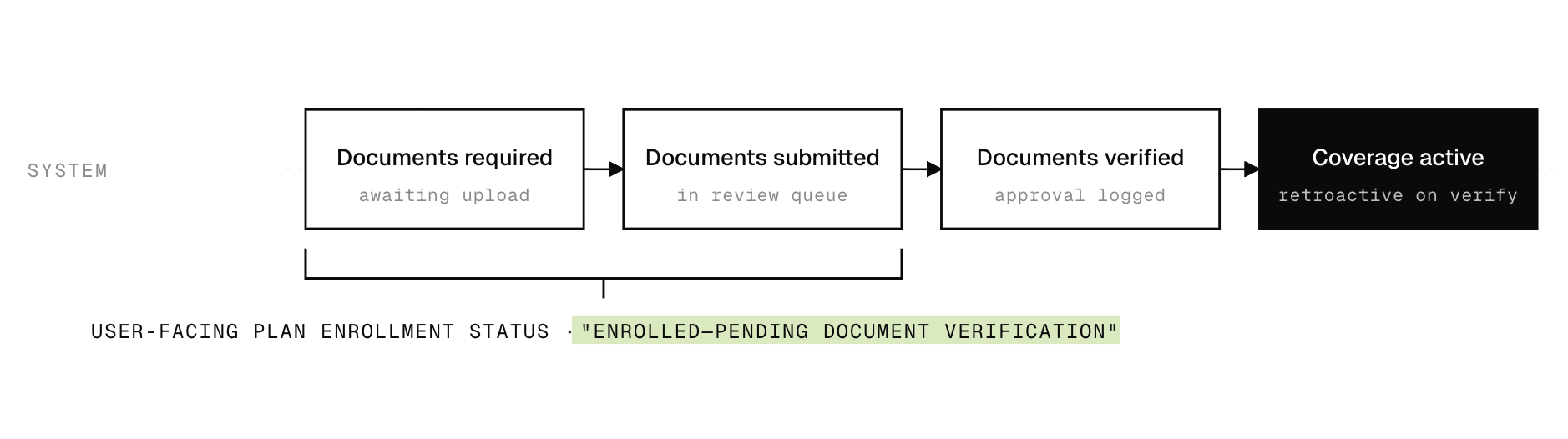
CONSTRAINTS & EDGE CASES
While conditional enrollment doesn't eliminate the coverage gap completely, it allowed people to plan for care sooner and accelerates coverage activation.
Conditional enrollment allowed customers can engage with their plan in advance and recover claims retroactively upon approval, rather than waiting in limbo for an Account Worker to approve first.
Some other edge cases we designed for:
-
Multiple qualifying events per household
-
Multiple documents per case
-
Document rejection and resubmission flows
-
When coverage should start
Working on this taught me that in complex and high-stakes systems, edge cases can make or break the design. So prioritize failure modes, downstream impacts, and constraints as first-class considerations.
This project taught me that design decisions extend beyond the interface into the broader customer journey. What appeared to be a simple flow change (uploading documents) surfaced policy questions no one had anticipated – like whether enrollment could be conditional, how payment should be handled, and what the user sees.
OUTCOMES & LEARNINGS
Customers received health coverage sooner
Conditional enrollment let customers enroll and pay immediately, with coverage activating automatically upon verification
Streamlined document processing
Reduced document processing time from months to days, reducing the coverage gap for customers experiencing life changes
Zero high-impact
defects
Thorough edge case planning, downstream impact analysis, and testing ensured a stable system to 1.5M+ residents with no p0/p1/p2 issues
For more information on this project, please reach out.
A smart journal that acts as a digital mirror and emotional companion